Women aren’t heard in healthcare, and that’s just the beginning
By Sophia Ketterer
Mia Elias’s father is welcome at the hospital. She is not.
“It was in that moment where I really realized they don’t give a fuck about women’s health,” said Mia Elias, a woman who has repeatedly had negative health care experiences.
Elias is a 21-year-old who was diagnosed with Poly Cystic Ovarian Syndrome at 14, and later with endometriosis.
“They don’t want to explore it and they don’t want to understand it and they dismiss it. It’s not even just doctors. So many people just don’t take women’s health seriously,” she said.
One of the root causes of this issue is the lack of research done on women’s health.Before 1993, women were largely excluded from clinical trials. Women are twice as likely as men to experience adverse drug reactions, in part because many drug dosages and trials were conducted primarily on men. Even in studies on mice, many medical researchers avoid using female mice due to perceived higher costs and concerns that fluctuating hormones and reproductive systems might “confound” results- a belief that has been scientifically proven to be incorrect.
View this post on Instagram
Many women, like Elias, have received unfair treatment from doctors. Because of their experiences, many have taken to social media to find a community or get the advice their doctors don’t provide to them.
Platforms like Instagram and TikTok are filled with creators giving out “health and wellness” and medical advice. This causes users to be inundated with information they might not want or need. Much of the information is false, but it can be hard to tell what’s accurate and what’s not. There are no regulations on who can share health information online, and the lack of transparency and strict guidelines make it even more confusing.
For example, many creators claim to be nutritionists without any official education. Anyone can legally call themselves a nutritionist, as there are no requirements or certifications for the title. Health and nutrition information could be coming from a nutritionist who’s never taken a single nutrition class or one who holds a PhD, and social media users often can’t tell the difference.
There are non-dietitians telling people what to eat, non-personal trainers giving out workout plans, and non-doctors telling women how to “heal their hormones naturally.”
Kailee Bryant is a 21-year-old who has experienced the detrimental effects that social media health information can have.
“For me, the basis wasn’t, ‘oh, I need to lose weight.’ It was, ‘I need to eat the healthiest and cleanest, whatever clean means,’ that I can and be the healthiest version of myself. And that’s where TikTok came in,” said Bryant.
“I feel like young girls especially are so susceptible to that kind of information. And it’s not like they’re looking to see, ‘oh, is she a certified dietitian? Is she a nutritionist?’ They see one video saying that to balance your hormones you need to eat no carbs, and then they think, oh, wait, I’m not supposed to eat any carbs. And then it can completely destroy their health,” she said.
There are also a lot of men giving female health care advice on social media.
“I’ll see men [on social media], who are like, ‘How to get your period back as a woman.’ And, what do you know? Sure, you can do the research and stuff like that. But what connection do you have to womanhood? None,” she said.
“It’s always men telling the story and not incorporating the needs of women,” said Bryant.
“My doctor was also POC, so I feel like that was supposed to gain this trust and transparency between people and the medical system, but I would go to the doctor and explain my symptoms to her and I feel like she wouldn’t even listen to me. She would tell me ‘I think it’s all in your head. I think it’s anxiety,’ things like that. As a kid, that kind of just makes your trust go down in the system, because it feels like you’re not being heard,” said Bryant.
What her doctor told her was anxiety, was in fact not anxiety. She ended up being diagnosed with SIBO (small intestinal bacterial overgrowth).
While she’s experienced the negative effects of social media for health information, Bryant has also experienced the positive effects.
“As someone who’s in Generation Z, I did use TikTok to search up my symptoms, and I found that a lot of my symptoms were aligned with SIBO. I told my doctor, did a test and I did have SIBO. It was kind of dismissive, because again, my doctor was telling me that basically all my symptoms weren’t true, and then I did actually end up having something,” she said.
What her doctor told her was anxiety, was in fact not anxiety. She ended up being diagnosed with SIBO (small intestinal bacterial overgrowth).
While she’s experienced the negative effects of social media for health information, Bryant has also experienced the positive effects.

“As someone who’s in Generation Z, I did use TikTok to search up my symptoms, and I found that a lot of my symptoms were aligned with SIBO. I told my doctor, did a test and I did have SIBO. It was kind of dismissive, because again, my doctor was telling me that basically all my symptoms weren’t true, and then I did actually end up having something,” she said.
“My doctor was a woman as well, but I feel like maybe this is just an education issue itself. They’re not really prioritizing women’s health,” she said.
Kailee Bryant. Photo Credit: Kailee Bryant
This lack of proper listening and care is happening at the same time that women’s health, both in medicine and in culture, continues to be misunderstood and undervalued. Women have historically been silenced and dismissed in healthcare. They are not taken as seriously as men and frequently do not receive the same quality of care.
“I went to so many doctors and they didn’t know what was going on,” said Elias.
“I would literally fall to the floor from the pain. I went to the hospital once, and the male doctor said, ‘these just sound like normal pains.’ I told him, ‘this isn’t normal.’ After scans came back clear — because endometriosis can’t be detected on scans — he said, ‘hospitals are for emergencies, not for women’s issues.’ Then he gave me Tylenol and told me not to come back unless it was a real emergency because it wastes their resources,” she said.
Elias was left in her hospital bed crying because she didn’t know what was wrong with her and she was being dismissed by numerous doctors and no one was helping her. Her primary care physician told her that it was just her anxiety.
Just a few months later, Elias witnessed firsthand the disparity between how men and women are treated in health care. Her father had really bad acid reflux along with really bad chest and arm pain. Concerned he was having a heart attack, she drove him to the hospital.The doctor came out and it was the same doctor she had when she was there a few months prior.
“He doesn’t recognize me, obviously. They rule out a heart attack, do a chest x-ray and some other things. He looks at my dad with full sincerity and says, ‘sir this is what we are here for. You come any time; it’s why we’re here. This stuff happens all the time. I’m just glad you’re okay,’” said Elias.
Elias had to miss 171 classes during her senior year due to pain from endometriosis. When she met with her dean about it, he brushed her off, saying, “We all get a little stomach ache sometimes.”

Mia Elias. Photo Credit: Mia Elias
Dr. Marcia Ciccone is an assistant professor of clinical obstetrics and gynecology and the fellowship program director for gynecological oncology at USC Keck School of Medicine. She said that we have significantly less scientific data on conditions that affect women versus conditions that affect men.

“Things like PCOS and endometriosis and menopause. These are all things that I think doctors tend to overlook and not treat as much. Treatments for women’s health issues are not coming out as fast and there isn’t as much money on a societal level that’s being invested on those types of projects,” said Ciccone.
Dr. Marcia Ciccone. Photo Credit: USC Keck School of Medicine
In a study done on gynecological patients and their use of social media for women’s health information, the survey found that 57% of the women use social media to learn about women’s health. It also found that 92% of women believe that women’s health information should be available on social media, and 59% find it helpful in making health decisions. These women also used social media more for health information specifically around doctors visits.
“It’s common for people to start digging into the internet and self-diagnose when their doctor’s not giving them the answers,” said Cicone.
“Theres definitely a lot of medical gaslighting that goes on” she said.
Thirty-year-old Danielle Majewski experienced that gas-lighting for six years.
She started having symptoms in her vagina that were really painful and uncomfortable and affecting her daily life. She had only had sex with one person at that point and it was a woman. She has never had sex with a man. She decided to go see a gynecologist. She saw a male gynecologist, who she said had no bedside manner at all.
“He looked and examined me. He did not make me feel comfortable, didn’t talk me through anything. He asked, ‘When was the last time you had sex?’ I said, ‘Well, this week, but, it was with a woman,’ and he responded with, ‘no, when was the last time you had sex with a man?’ And I said, ‘well, I haven’t. I’ve only had sex with women.’ He then looked at me and his direct quote was, ‘I’m your doctor. You don’t have to lie to me,’” said Majewski. “He couldn’t conceptualize that a penis has never been inside me.”
“He told me, ‘you have an STD.’ And I was like, ‘okay. well, how? Is this something that could be transferred from a woman?’ And he goes, ‘no, from a man, that’s how I know you’re lying to me.’ He was being so aggressive, literally telling me that I was lying to him about having sex with men when I wasn’t,” she said.

Danielle Majewski. Photo Credit: Danielle Majewski
He then proceeded to diagnose her with an STD called Trichomoniasis. He then told her he had to biopsy one of the cuts to test for it.
She was terrified and was hysterically crying. He biopsied the cut, which she said as the most traumatizing experience of her life. The test then came back negative because she did not have the STD her doctor claimed she did.
She decided to never go back to that gynecologist, and saw a different one next. He was also a man. He also told her it was most likely an STD or a bacterial infection from a man. So, she went to another. He was also a man.
“I was gaslighted by three separate male gynecologists, board-certified male gynecologists, telling me that I was lying about having sex with men. Because obviously my issue was an STD, and it never was,” she said.
“So that was from 2017 to right before COVID. I think January 2020 was when I saw the last male gynecologist, because the cuts never went away. No one ever gave me an answer. And the only answer I ever got was that I was this from a penis, which was literally impossible,” she said.
Majewski saw her first female gynecologist in 2021 and was asked the same question, if she was having sex with men. The doctor thought it might be bacterial so she prescribed Majewski numerous creams, gels and suppositories. She used them for the next three years and nothing helped. In fact, her symptoms actually got worse. She had trouble walking and was bleeding.
She then saw a gynecologist in Pennsylvania, where she lives, who Majewski said took 20 seconds to diagnose her with a skin condition called lichen sclerosus.
“I told her all of my stories, and she cried with me because she was like, ‘I can’t believe that you were treated that way.’ And I was like, ‘nobody listened to me. Nobody believed me.’ I wasn’t having sex like crazy, and I was just gaslit and mistreated,” she said.
“The craziest part about it was all of the male doctors accused me of lying about having sex with men, and I thought that was the weirdest thing to say. Even when I said, ‘no, my partners are women.’ They’re like, ‘have they always been women?’ They wouldn’t just take it for what it is,” she said.
Another major topic in women’s health is birth control. It is often prescribed by doctors as the only solution for a range of women’s health issues, without offering or discussing alternative treatment options.
Photo Credit: Sophia Ketterer
“I don’t know that that’s a normal understood thing from most doctors,” said Ciccone.
“I try to advocate for this a lot. Patients need to understand what’s going on with them. You can’t just tell them ‘oh, you have this,’ and then let them go out into the world and deal with it. You need to explain to them why that happens, what their different options are and then people can make their own decisions. Part of avoiding people having misconceptions from the internet and social media is having a conversation with your patient and making sure they understand what’s going on with them,” she said.
Elias dealt with this concept of her pain not being easily seen or fixable. Even when she was falling to the floor, crying in pain, doctors tried to write her off.
“People with chronic pain tend to be annoying to their doctors because they have a problem that they can’t really fix. Especially when it’s something the doctor is unfamiliar with, especially if it’s a male doctor or an older doctor,” said Ciccone.
Alexandra Donovan is a 23-year-old who considers herself to be one of the healthiest people she knows. She eats well, exercises regularly and tries to go to bed by 10 p.m. She had already been diagnosed with SIBO when, the year before college, she began getting severe acne. After trying everything, she went to a gynecologist. The solution? Birth control. She was diagnosed with PCOS and was told it was her only option.
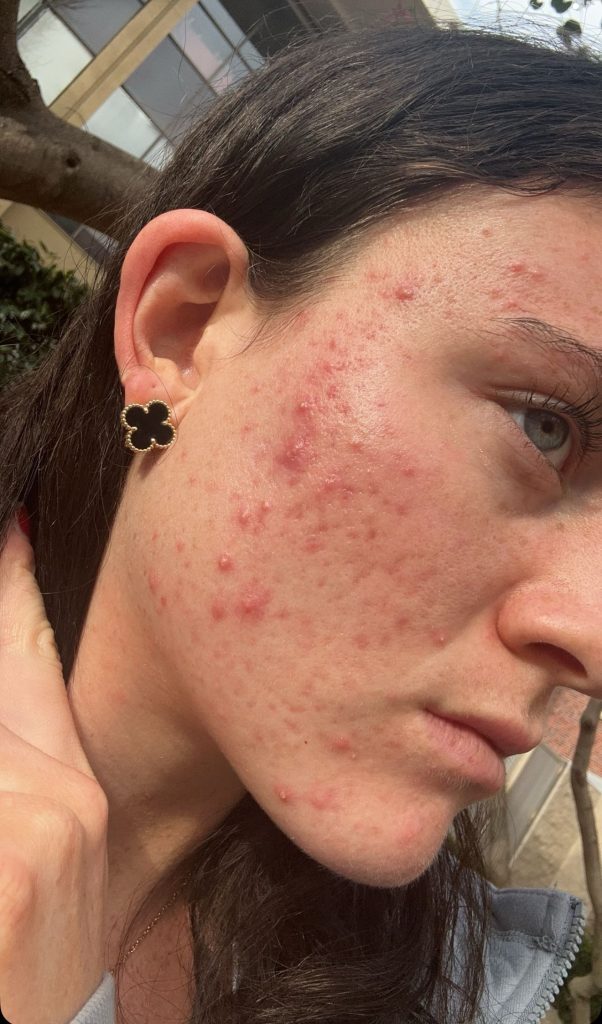
“It’s disheartening because women in our medical system just aren’t taken care of the way they need to be and aren’t researched properly,” said Donovan. “A lot of times I was just told to eat less and work out more, and that doesn’t work for people with hormone disorders.”
That advice is also simply dangerous.
“It took me probably five years to get a diagnosis and they’re now pushing me in the direction of autoimmune disease,” she continued. “It’s been a really long journey of me chasing my tail, and I’ve used a lot of social media to figure out what I had based on what I’ve seen online. I get a lot of my hormone advice from people on TikTok. I’m cautious about what advice I take, but I think social media has been really helpful for me.”
Alexandra Donovan. Photo Credit: Alexandra Donovan
Aside from the gender bias that has been ever present in healthcare, there is also systemic racism in the system. According to the Kaiser Family Foundation, “Black women who are younger and with self-reported darker skin tones are more likely than their counterparts to report preparing for possible insults and being careful about their appearance during health care visits.”

Maternal mortality is an epidemic. In 2023 alone, about 260,000 women died during and following childbirth, according to the World Health Organization. The same report also found that over 700 women died from preventable causes relating to pregnancy and childbirth every single day. Nearly every two minutes in 2023, a maternal death occurred. About 84% of these deaths are considered preventable.
The statistics for Black women are even worse. Pregnancy-related mortality is about four times higher for Black women than it is for white women, according to the Mayo Clinic.
This bias partially stems from some health care providers who hold false beliefs about biological differences between Black and White individuals. These misconceptions suggest that Black people have less sensitive nerve endings, thicker skin, and stronger bones. Such false beliefs lead many health care providers to underestimate Black patients’ pain and provide less appropriate treatment.
“There was a lot of discussion in more recent past years about gender bias, racial bias, all this stuff that goes with microaggressions. Whether it’s bias against women, bias against somebody’s ethnicity, whatever it is [one has] to be aware of this. So you won’t be giving people bullshit ass advice because you’re angry and you’re racist or whatever it is.” said Dr. Gregory Taylor is a clinical associate professor of medicine and medical director of the Keck Signature Care Program, which is a concierge medicine program.
Unlike many females, Dr. Talyor can’t remember a time women were treated differently in his own experiences. Perhaps, because he is a man. He is aware the bias exists, however.
“Obviously I’m not a woman, and I don’t go to the doctor’s office with my wife. I have a daughter and on occasion, I go to the doctor’s office with her…. I don’t remember at least off the top of my head to give you any examples of women being, I guess, neglected or dismissed as a medical student. I just don’t recall that right now. But all that being said, I do hear stories or I’ve heard instances that women are often unheard and have not been given the proper amount of respect in the healthcare setting. So I don’t disagree with that. And I think that’s a bad thing overall,” he said.

Dr. Gregory Taylor. Photo Credit: USK Keck School of Medicine
In the United States, most high schools only require one semester of a general health class in middle or high school. Criteria is not nation-wide and varies by state. Classes like anatomy and physiology are not required, so people are often left unaware of their own bodies. Only37% of U.S. states require sexual education in schools to actually be medically accurate.
These issues that women and other minority groups face stem from early on in life and education and are engrained in society from the start. Similarly, only four states require sex education to instruct on menstrual health beyond teaching about puberty. Young girls are set up to be uninformed or misinformed about their bodies, leading to health disparity issues in the future.
Dr. Jerry Abraham is the President of the Los Angeles County Medical Association and currently serves as the Director of Integration & Public Health at Kedren Community Health Center. Dr. Abraham also serves on the faculty of the USC Keck School of Medicine Public Health Program and the UCLA David Geffen School of Medicine Urban Health Equity Pathway.

Photo Credit: USC Keck School of Medicine
“There are a lot of health disparities. Period,” said Abraham.
“What makes a bigger impact on our health? Is it our zip code? Does our gender, sex, orientation, whatever other persuasions are, race, ethnicity, age, these are all things that we can slice and dice and really drill down into understanding why we see different groups faring differently,” he said.
Regarding social media for medical advice, Abraham says it’s an educational issue.
“At the bottom of a lot of this is, why are we not learning more about our bodies and who we are in middle school and high school? We shouldn’t wait to go to medical school to take anatomy and physiology and know how our bodies function,” he said.
He is also concerned with how and where people are getting their medical information from.

“The misinformation, disinformation is rampant… we’re seeing it from the highest levels, from the president’s office all the way down… it’s so sad that right now we can’t go to our Centers for Disease Control and Prevention, which should be the trusted voice… it’s definitely getting harder to figure out who to trust and what’s accurate… even as a physician, I’m getting nervous about the types of things I’m finding when we search for the way AI is being used… we’re dealing with a runaway train, and we are not ready for it,” he said.
Dr. Jerry Abraham. Photo Credit: National Medical Fellowship
“The point of the story is poor folks are not doing well in this country… I’m going to really focus in right now on Black and brown patients and women… This administration has been devastating for women’s health,” said Abraham.
Abraham feels like we are moving back in time as a society when it comes to diversity, equity and inclusion.
“On top of all the insurance challenges that we’re seeing, of course, all of the attacks on DEI are devastating and damaging. We are trying to navigate how to continue to train doctors in medical schools here at UCLA, USC, and Charles Drew Kaiser Permanente. How do we do these things if we’re banning the words like ‘DEI’ and ‘health equity?’ So we need to understand why there are disparities and why black women suffer higher complications during pregnancy, including death,” he said.

These issues that women and other minority groups face begin with what we’re not taught and continue in what the healthcare system still refuses to learn, leaving generations of women to navigate care that was never built with them in mind.
Elias’s father was told the hospital was there for him. Women, both explicitly and implicitly, are continuing to be told that healthcare is not there for them. Until this changes, this will remain a tragic story that never ends, with no ending in sight.
**art by Sophia Ketterer
